There has been a wide range of advice on indoor air quality (IAQ), carbon dioxide (CO2) monitors, air cleaners/purifiers and HEPA filters circulating from COVID-19 pandemic times. Much of it centres around living with COVID-19 and trying to make our classrooms, offices and other workplaces, safer environments.
We are also looking to the future and operating with greater protection measures against airborne pollutants and virus particles.
Airborne pollutants and virus particles
COVID-19 and other pollutants – that are most damaging to human health – are airborne. They are so small that they’re invisible to the human eye and are spread through the air by aerosol, emitted when speaking, coughing or sneezing.
COVID-19 has the potential to spread by aerosol at both long and – more likely – short range. However, given favourable conditions, smaller virus particles – attached to aerosols – can spread over a long range, i.e. a distance of more than two metres and can remain suspended in the air for hours. For that reason, there is an added emphasis on ventilation – a tool to help clean the air and make indoor environments safer for occupation.
Inadequate ventilation
As a visual, the behaviour of cigarette smoke in an indoor setting is a good substitute animator for airborne pollutant or virus particle spread – filling a space, lingering for hours and infecting those around. With that in mind, it is not hard to see why buildings or rooms without adequate ventilation are among the riskiest environments, when it comes to pollutant or virus spread.
Surface to air – a shift in emphasis
There was a shift in emphasis during the COVID-19 pandemic from cleaning objects and materials, known as fomites – to cleaning the air. Epidemiological data and studies of transmission show the risk of fomite infection to be low. However, it is wise to clean and disinfect any indoor community areas where a confirmed case or a suspected case has occurred within the past 24 hours.
The British Medical Journal (BMJ) states:
“the transmission of SARS-CoV-2 after touching surfaces is now considered to be relatively minimal”.
While the Centres for Disease Control and Prevention (CDC) states:
“infection via the fomite transmission route is low, and generally less than 1 in 10,000”.
Emphasising hand hygiene and respiratory etiquette, however, should continue. Proof that the coronavirus is airborne has brought air quality into focus and shifted the emphasis to tools that could boost indoor air quality, like ventilation.

Indoor air quality (IAQ)
With the majority of our lives spent indoors – on transport, at home, working and sleeping – the provision of safe indoor interactions are key in living a healthy life.
To understand indoor air quality we must first recognise the role of ventilation.
Ventilation is the introduction of fresh outdoor air into a building or space to vent, replace and clean the indoor air. The goal of ventilation is to deliver fresh air for the breathing health and comfort of occupants. In other settings, the goal of ventilation is to rid the air of smells and odours, where for example, cooking or chemical processes are taking place.
This delivery of fresh outdoor air makes ventilation an essential tool in preventing the spread of airborne pollutants and virus particles, such as, COVID-19. Therefore, a ventilation strategy should be put in place for each indoor space, using a risk-based approach for specific activities, as some activities – such as singing – generate more aerosols than others.
The benefits to better indoor air quality are clear and obvious. Good indoor air quality:
- Reduces the risk of virus spread.
- Assists lungs in functioning better.
- Lowers medical costs.
- Improves the productivity of occupants.
It is clear that to provide safe indoor spaces, ventilation is essential, so how much ventilation is required?

Ventilation and air changes per hour
Ventilation – mechanical or natural – is supplied at a ventilation rate. The ventilation rate is the number of times the air in a building or room is changed each hour. It is measured using the air change rate in air changes per hour (ACH). There are set minimum ACH rates for each building or room type, depending on the intended purpose or activity.
While there are minimum rates, specific ACH rates can be calculated by an engineer, taking into consideration, room size, number of occupants, location, exposure and the activity. It should be noted that due to air mixing, achieving ACH rates does not mean all of the original air is replaced.
Air supply rates
The below table shows examples of suggested fresh outdoor air supply rates per person – to achieve minimum ACH – from the Chartered Institute of Building Service Engineers (CIBSE). The rates are expressed in litres per second (l·s-1) or more simply l/s.
| Building/room type | Suggested fresh air supply rate |
|---|---|
| Office | 10 l/s per person |
| Hotel bedroom | 10 l/s per person |
| Hospital ward | 10 l/s per person |
| Teaching space | 10 l/s per person |
Any space that regularly contains multiple occupants is often the most poorly ventilated, frequently supplying below 5 l/s per person. Similarly, superspreading virus events are generally found to have very low air supply rates of only 1 to 2 l/s per person. Therefore, providing suggested fresh air supply rates can lead to safer indoor environments, reducing the risk of airborne pollutant or virus particle spread.
Air supply rates and productivity
Clean air can increase productivity. In showing a direct correlation between clean air and productivity, a field study in a US school displayed a mean 0.5% increase in maths scores for every 1 l/s increase in the air supply rate to a room.
Parts per million (PPM)
Generally, air supplied at 10 l/s per person equates to a carbon dioxide (CO2) concentration of around 800 to 1,000 parts per million (PPM) in an indoor setting.
PPM is a dimensionless quantity, which gives a good indication of room occupancy, as a result of measuring exhaled CO2 from persons present.
High PPM readings can be viewed as a warning of the potential build-up of environmental contaminants – such as airborne pollutants or virus particles – from persons present. For example, during the COVID-19 pandemic, at times of high community virus transmission, high PPM readings warned of potential risk to occupants.
PPM is generally seen as a good alternative for IAQ measurement, however, it should not be viewed as an absolute indicator of pollutant or virus infection risk.
Carbon dioxide (CO2)
CO2 is an odourless and colourless gas, produced from amongst other things, human respiration. CO2 is measured in parts per million (PPM), not to be confused with planned preventative maintenance.
Its presence gives an indication of occupancy in a room or space.

Carbon dioxide (CO2) monitors
CO2 monitors are devices that monitor the level of carbon dioxide in indoor environments, such as, schools, offices, hotels and restaurants. They can provide useful information – which can ultimately inform on a ventilation strategy – through analysis of a monitoring device’s historical readings.
A CO2 monitor will not inform on virus presence or concentration, it merely notifies of the presence of exhaled CO2. It does expose poorly ventilated indoor spaces. However, a low CO2 level does not always indicate good ventilation, as the low rate could be due to low occupancy.
Most monitors are employed in a building’s controls strategy integrated with a building energy management system (BEMS), as they call on mechanical ventilation or to activate motorised windows to introduce fresh air. However, during the times of the COVID-19 pandemic, CO2 monitors were also deployed to warn against poor air quality, where no mechanical ventilation existed. These monitors were generally standalone devices.
CO2 monitors are particularly relevant in areas occupied by groups of people for periods of more than one hour, like offices and school classrooms, which frequently record PPM readings of 1,500 or higher.
Considering outdoor PPM levels are 400 to 450, indoor PPM levels of 800 are considered well ventilated settings.
CO2 monitors and BEMS safeguard
Where mechanical ventilation and a BEMS are present, CO2 setpoints should be set to around 400 PPM; while during COVID-19 times, occupancy sensors that modulate fresh air supply should be disabled to boost ventilation.
Depending on specific equipment and the site setup, additional safeguards can be put in place to boost ventilation. Alerts – communicated by email or text message – can warn building occupants to increase ventilation by natural means – if the CO2 monitor or sensor warns of inadequate ventilation. This is performed via a BEMS.
Standalone CO2 monitors
>To obtain an accurate reading, monitors should be placed on an internal wall, at head height and away from people, fresh air inlets, cooking areas, fires and stoves.
Poor IAQ readings
The danger of poor indoor air quality exists in settings where high or enhanced aerosol creating activities are taking place, such as, gyms or theatres. Danger also exists in smaller spaces, even if operating at low occupancy and well ventilated.
Larger spaces are more favourable, although while PPM levels might be low, there is still no guarantee that airborne pollutants or virus particles are not present. These areas should increase air flow rates to 15 l/s per person, maintain CO2 levels at 800 PPM and consider reduced occupancy numbers and time.
PPM indicators
While there are no official thresholds to good or bad CO2 levels, the table below acts as a good indicator of normal, bad and potentially harmful PPM readings.
| CO2 level | Indicator | Status set |
|---|---|---|
| 400 to 800 PPM | Green | Normal |
| 800 to 1,000 PPM | Yellow | Warning |
| 1,000 + PPM | Red | Alarm |
In a study by Environmental Health Perspectives (EHP) in an office-like environment, it was found that performance diminished by 66 percent with a CO2 level of 1,000 PPM when compared with the same space at 600 PPM. In the same study, performance output reduced by more than 75 percent when CO2 levels reached 2,500 PPM, versus 600 PPM levels. Study results, therefore, show increased fresh air supply rates can productively and economically benefit workplaces.
Best performing CO2 monitors
When purchasing CO2 monitors, ensure to buy a non-dispersive infrared (NDIR), as they are specifically designed to detect carbon dioxide in a space. Other monitors containing equivalent CO2 (eCO2) sensors merely suggest CO2 levels based on room volatile organic compound, rather than reporting on actual levels. This NDIR CO2 monitor from Aranet is widely used and cost between € 200 and € 300.
A CO2 monitor’s performance can drift over time. Standalone CO2 monitors should be proven each week and re-calibrated – by removing the monitor and exposing it to outdoor fresh air. Monitors or sensors that are part of a mechanical ventilation system should be serviced in-line with the manufacturer’s recommendations.
When indoors, to obtain a valid reading, allow for readings across the space of at least one hour to gain relevant sample data.
Standalone CO2 monitors in schools
With every school in Ireland now in possession of a CO2 monitor, a ventilation strategy should be put in place. When deciding on a ventilation strategy for schools, the age of both students and the building should be considered.
Children aged between seven and nine years old produce roughly half the CO2 of a teenager. While newly built schools can typically suffer from under ventilation and overheating, with the opposite for older buildings.
The recommended fresh air supply rate in a school is at least 10 l/s per person. An engineer can advise on achieving this rate.
Thermal comfort
Without mechanical ventilation supplying and extracting air, achieving ventilation rates and providing thermal comfort can prove difficult. Particularly for those situated close to window draughts in winter time. Dress and clothing can help counter this issue.
Clothing can affect thermal comfort. Relaxing dress codes during colder winter months by allowing occupants to dress in warmer clothing can benefit thermal comfort.
Metabolic rates can also affect comfort, therefore, allowing and supporting breaks and regular movement away from desks can improve thermal comfort and aid health.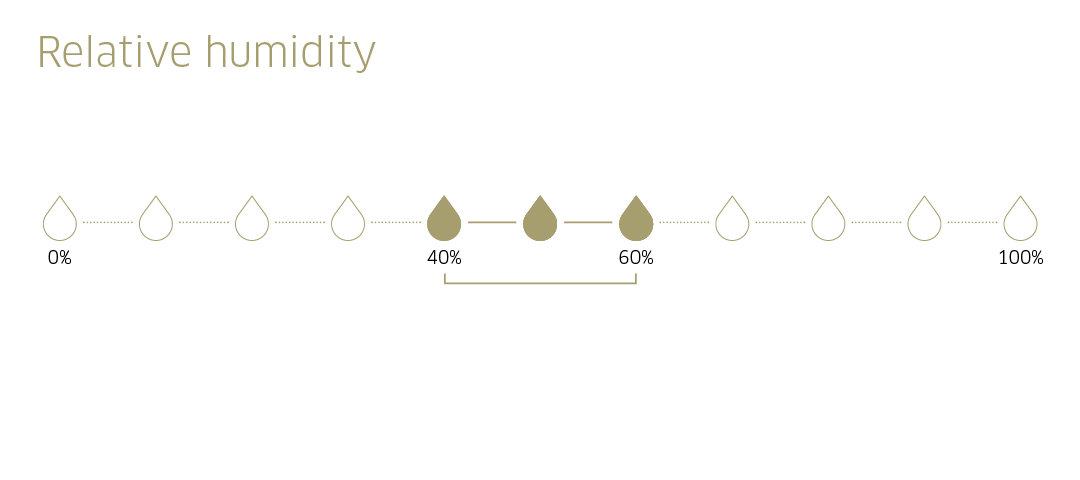
Relative humidity (RH)
Relative humidity can have an impact on IAQ, particularly dry indoor air. Where the control of relative humidity is possible in mechanical ventilation systems, it is recommended that levels of 40 to 60 percent should achieved. Keeping a minimum relative humidity value of 40 percent can reduce the impact of airborne pollutants, virus particles and other seasonal respiratory infections.
When relative humidity is less than 40 percent humans become more susceptible to viral outbreaks. This is because the reduced humidity in the air provides a clearer route for virus aerosols to travel longer distances. Also, in the dry air of lower relative humidity values – 10 to 20 percent – the ear, nose and throat are not as effective at filtering virus particles, as mucus becomes dry and more susceptible to infection, reducing the capability to block virus particles.
At less than 40 percent relative humidity, water in cough aerosols – to which virus particles attach themselves – begin to evaporate, leaving a much smaller droplet aerosol. As a result this aerosol can travel further and stay suspended for longer. This provides a risky environment for occupants. Conversely, at high humidity, of greater than 95 percent, with more moisture in the air, aerosol sizes can increase, providing a risk for those in the immediate vicinity of the droplet aerosol.
Maintaining relative humidity at 40 to 60 percent is the least risky option as not only are human defences functioning at their most effective, but a potential pollutant or particle will retain moisture, ensuring their hazard is not increased.
Boost IAQ
1. Focus on fresh air
Coronavirus and other pollutants that are most damaging to human health are microscopic and airborne. Just because they are out of sight, it doesn’t mean indoor air quality should go out of mind. Review ventilation means – be they mechanical or natural – and look at ways ventilation can be improved upon and – if necessary – increased. Know the suggested fresh air supply rate for your building and ensure fresh air is supplied, considering, the room size, activity, location and exposure.
2. Risk assess indoor environments
How many people will be attending? How long will they be in attendance? What activities will they be performing – will they be performing high aerosol generating activities, such as, exercising or singing? What type of ventilation is present to assist in in the delivery of fresh outdoor air?
3. Ventilation strategy
How is ventilation provided? If mechanical ventilation or air conditioning is present, is it provided in a way that won’t exasperate virus particle or airborne pollutant spread, especially at times when virus or seasonal illnesses are more prevalent in the community? With that in mind, advice on the configuration of mechanical systems and air conditioning units to minimise re-circulation, can be found in Thermodial’s HVAC systems safe operation guide.
CO2 monitors can assist in a ventilation strategy by uncovering areas of poor ventilation. Ideally, they should be linked in with a mechanical ventilation system, feeding data to a BEMS, however, a standalone monitor can assist in buildings with little or no mechanical ventilation.
Consider other measures, such as, physical distancing; reduced occupancy; natural ventilation and ways to aid thermal comfort; installing mechanical ventilation systems and relative humidity control.
Thermodial’s approach
While COVID-19 might be on the wane, variants of the virus could linger for some time to come. In addition, other harmful airborne pollutants that negatively affect indoor air quality will remain, such as, seasonal viruses, dust, fumes, smoke, spores and pollen. Therefore, a human-centred and risk averse approach is necessary to provide a safe indoor environment for staff, customers and visitors alike. Studies showing, increased air flow and lower PPM values can facilitate increased productivity, to the economic benefit of the workplace.
Thermodial engineers can review your current ventilation setup, taking a risk averse approach. They can identify areas of poor ventilation, advise on how CO2 monitors/sensors can be most effectively utilised and then, if required, carryout works to increase air flow rates in the safest, most cost and energy efficient manner.
Talk to Thermodial about ventilation services to support your businesses’ critical needs or explore our full capabilities in HVAC planned preventative maintenance and HVAC upgrades.
Key guidance source materials
Aerosol Air Quality Research – An Overview on the role of relative humidity in airborne transmission of SARS-CoV-2 in indoor environments
British Medical Journal (BMJ) – COVID-19 has redefined airborne transmission
Centres for Disease Control and Prevention (CDC) – Science brief: SARS-CoV-2 and surface (fomite) transmission for indoor community environments
Chartered Institute of Building Service Engineers (CIBSE) – emerging from lockdown: ventilation guidance (version 5)
Chartered Institute of Building Service Engineers (CIBSE) Journal – Improving air quality for education
Environmental Health Perspectives (EHP) – Is CO2 an indoor pollutant? Direct effects of low-to-moderate CO2 concentrations on human decision-making performance
Federation of European Heating, Ventilation and Air Conditioning Associations (REHVA) – COVID-19 guidance document (version 4.1)
Government of Ireland – Expert Group on the role of ventilation in reducing transmission of COVID-19: second report (02 March 2021)
Joint Oireachtas committee on health (Orla Hegarty) – COVID-19 prevention is possible by managing people and managing indoor air
Updated - download HVAC and water systems - safe operation guide [PDF - version 2]
This is a guidance for facility managers and building owners on the use of HVAC and water systems during COVID-19


